Knowing Me, Knowing You: What Can We Learn From Familiar Surgical Teams?
Incision · · 6 min readTeamwork is at the heart of a successful surgical procedure. Within seconds of stepping foot inside the OR, it is patently clear whether a team works well together — or it doesn’t.
In the first of this 2-part blog, we dive deep into surgical teamwork to uncover new perspectives on team familiarity. What benefits come with more consistent and familiar teams? And what lessons can we take from these to improve and support our own?
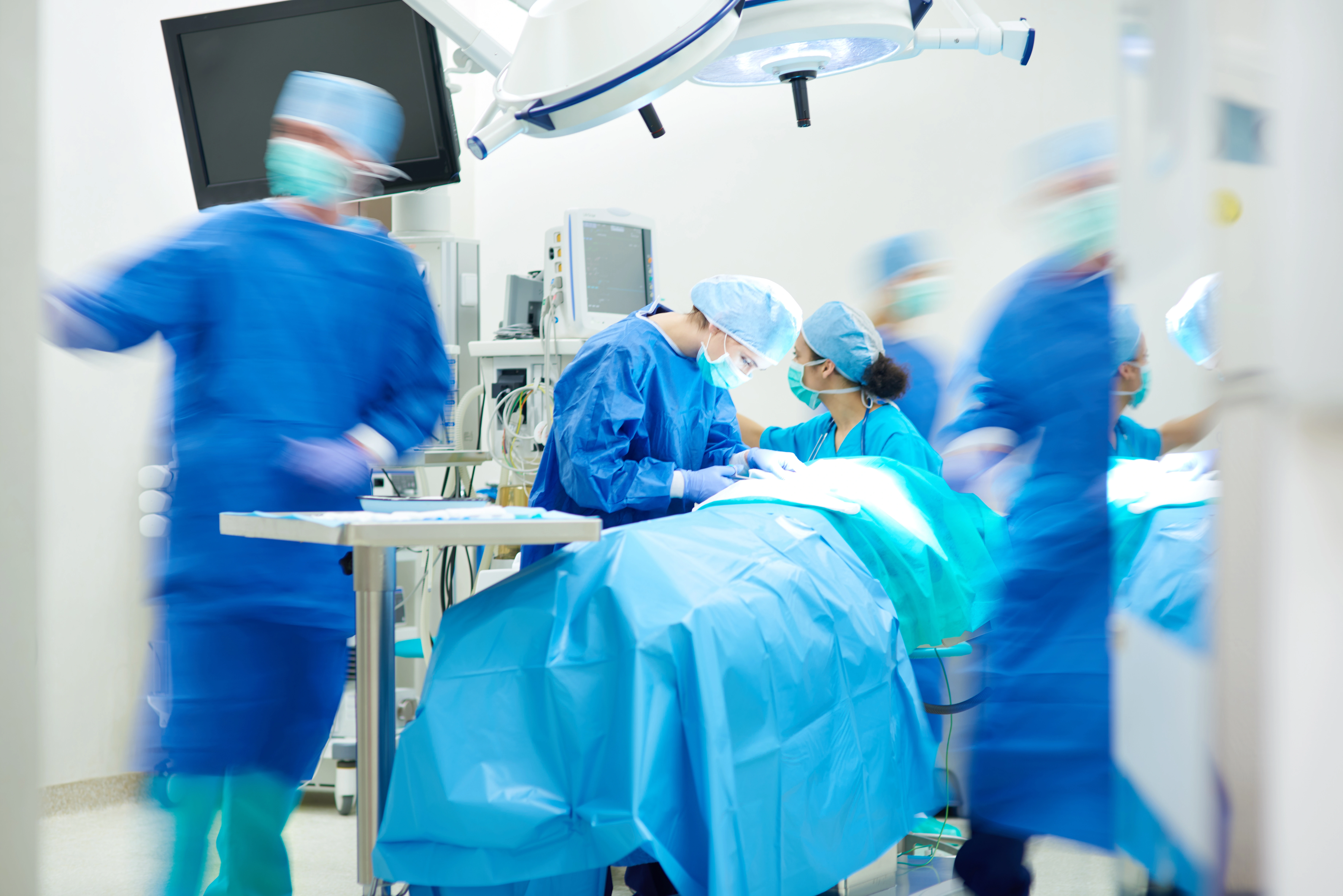
What’s a Familiar Team?
Surgical care is the product of numerous interprofessional interactions, reflected in several key multidisciplinary teams. In the operating room (OR), the team responsible for the delivery of a procedure is typically a combination of surgeons, nurses, anesthesiologists, and technicians working together on a shift-based and/or specialty-based rota. Work in the OR involves highly adaptive and task-focused collaboration between team members, often around safety-critical protocols and sophisticated equipment; intuitively, it makes sense that a history of working together would be helpful.
This property of a team — members having some degree of prior experience working together — can be referred to as its “familiarity.” Teams formed of individuals who have worked together a lot (for several months, or perhaps years) have a high degree of familiarity. Research from fields as far-flung as software development, police training, and human resource management shows that higher levels of team familiarity are frequently linked to better results [1, 2, 3].
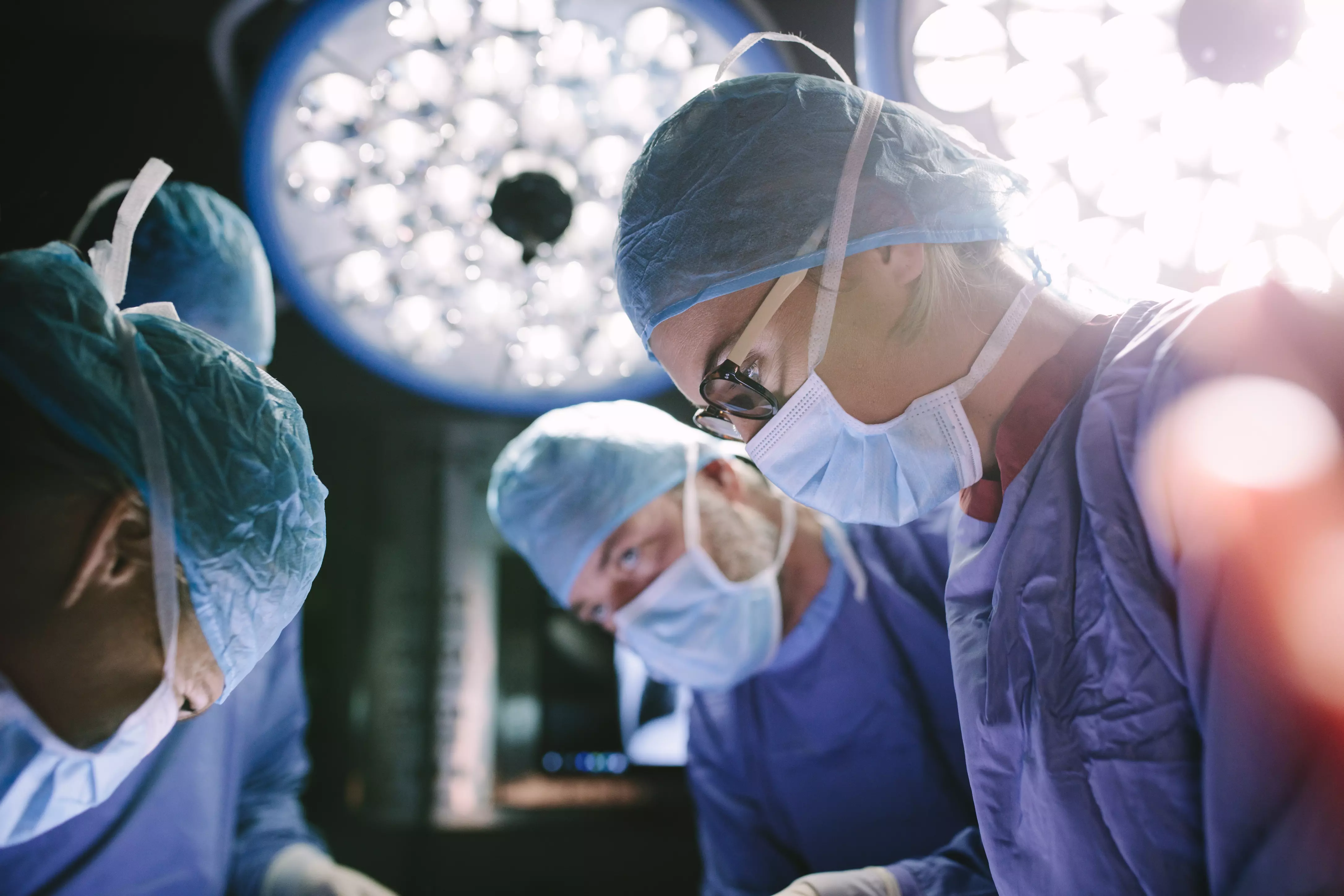
A growing body of research has identified team familiarity as a consistent driver of improved performance and better outcomes in the OR.
Faster and More Efficient
In 2022, a systematic review published in the Annals of Surgery examined the impact of team familiarity on OR efficiency [4]. Researchers from the University of Chicago found that the strongest impact of more familiar teams was in decreasing operative times. Studies included in the analysis reported reductions of between 8% and 16% when teams were more consistent and members were more familiar. This depended on several factors, including the complexity of the surgery and the specific measures of familiarity used. In gynecology, more familiar teams have saved about 25 minutes per robotic-assisted sacrocolpopexy compared with less familiar teams [5]. For spinal fusion procedures, time savings as high as 91 minutes have been reported [6].
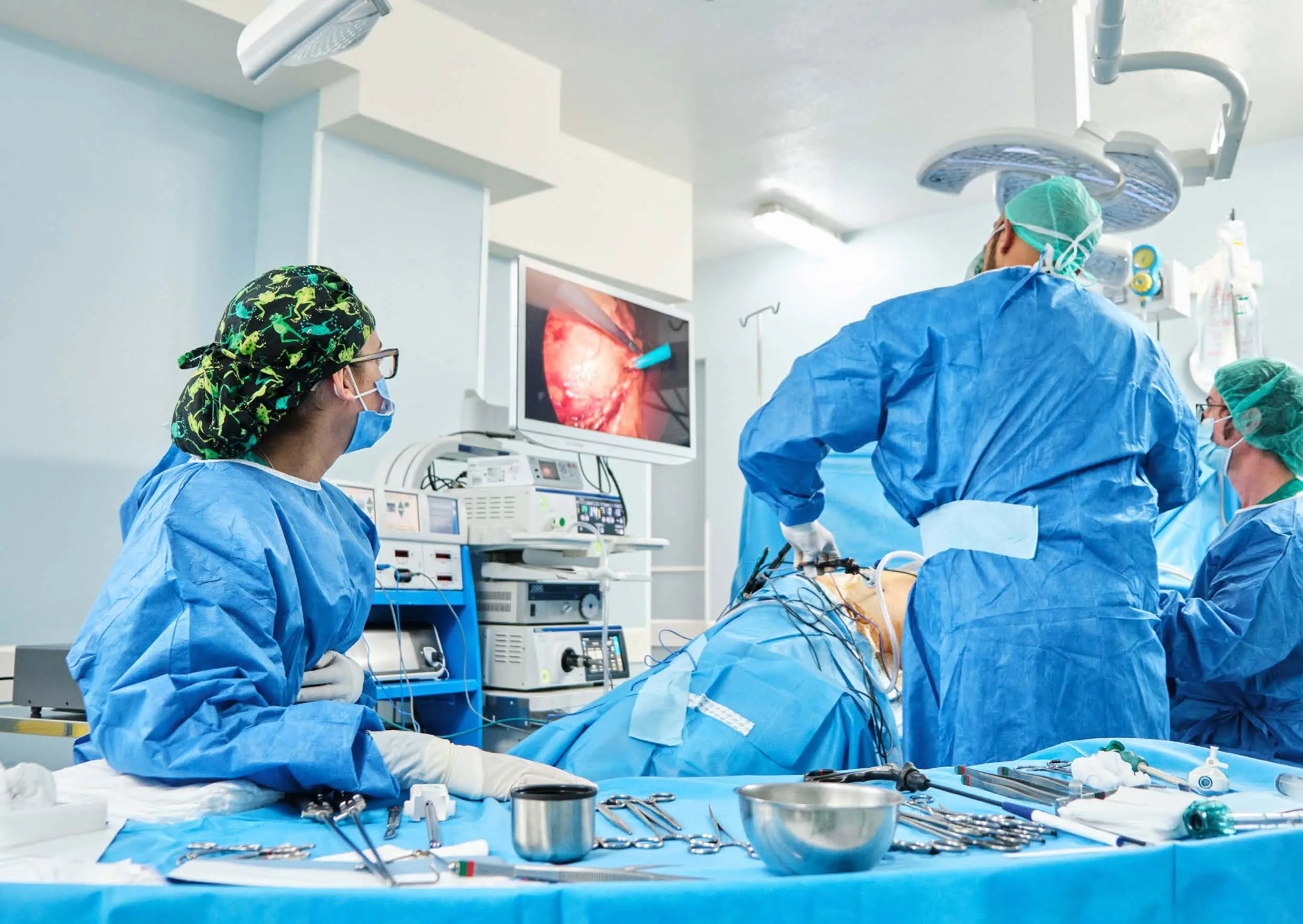
Increased familiarity is associated with better team performance, particularly in reducing operative time.
As well as operative times, familiar teams can improve OR preparation and turnover between cases. In general surgery, more familiar teams have demonstrated an 18% improvement in turnover time for inguinal hernia repairs and a 16% improvement in turnover time for laparoscopic cholecystectomies [7, 8]. The presence of a dedicated laparoscopic team (vs. a non-dedicated team) was shown to reduce total anesthesia time by 30 minutes, with significantly fewer delays related to setting up equipment [9].
Similar benefits appear consistent across specialties. In cardiac surgery, teams that routinely work together experienced fewer disruptions, errors and teamwork failures [10]. Neurosurgical teams reported fewer workflow disruptions in teams with high levels of surgeon-scrub nurse familiarity [11]. In urology, greater familiarity was associated with fewer “inconvenience events” in robot-assisted prostatectomy [12].
Better Clinical Outcomes?
As we’ve seen, improving OR team familiarity demonstrably increases operative efficiency. The relationship of familiar teams to direct clinical outcomes is less clear-cut. Less familiar teams have been associated with longer postoperative hospitalization in both cardiac and orthopedic surgery [12, 13]. In primary hip and knee replacement, inconsistent surgeon-nurse teams were associated with slightly higher rates of readmission (13.2% vs 10.0%), longer operative times, and a longer hospital stay.
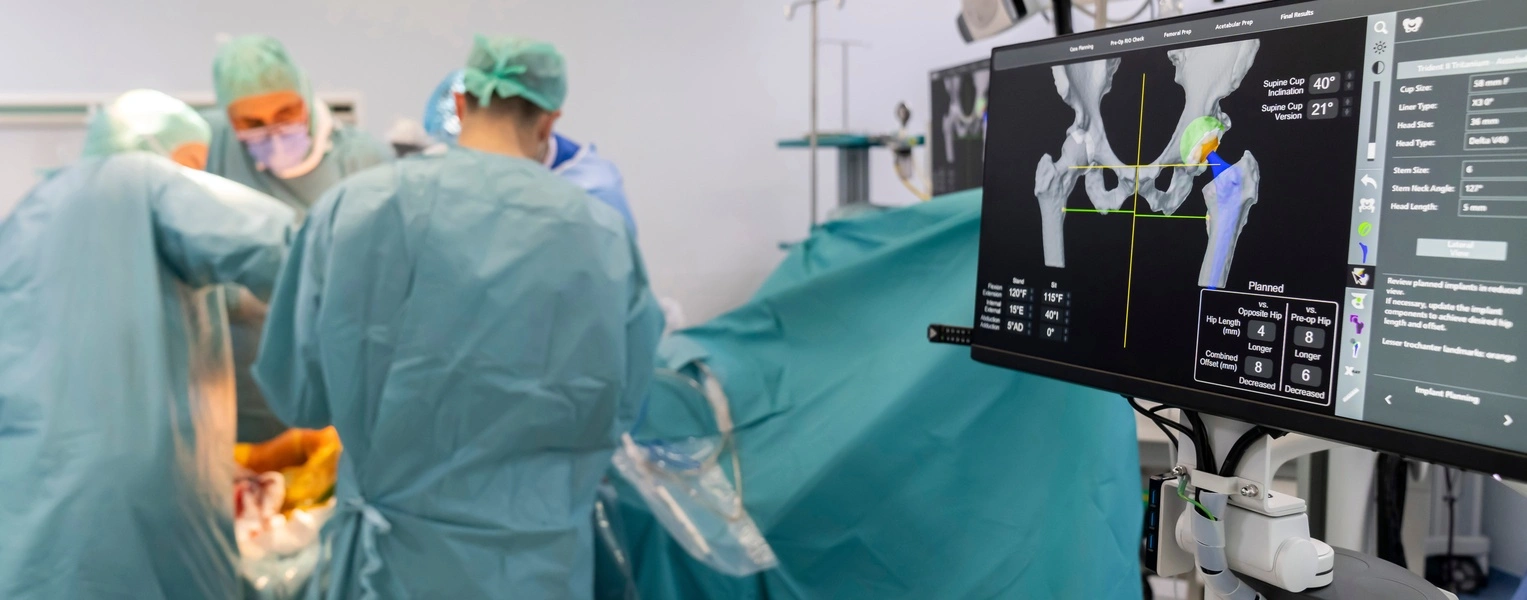
In breast reconstruction, one study identified an increased risk for reoperation due to higher rates of surgical site infections in less familiar teams [14]. Reoperation rates were significantly higher for attending surgeons with less than 150 prior case collaborations than those with more than 300 case collaborations. Other studies have failed to identify a significant link between familiar teams and reduced complications [15].
Complex Logistical Challenges
The superior properties of familiar teams are now fairly well established in surgery. This begs the question: how can we leverage these benefits to improve our own care provision? In practice, the biggest blockers to this are the logistical ones.
In a healthcare unit, shift patterns often prevent the formation of consistent operative teams — routinely bringing unfamiliar professionals together to fill rotas and maintain services. Rotating training programs create regular influx and outflux of surgical residents and trainee nurses. Understaffing and emergency cover create conditions where staff are often forced to work outside the teams they are used to. OR nurses, for example, typically have specialty-specific experience and yet are regularly required to work outside of their usual areas while on call or filling in for staff absences. Surgical managers are frequently required to form ad hoc teams with members who do not work consistently together.
There are significant logistical challenges to forming consistent and familiar teams.
These pragmatic challenges also pose an opportunity for innovation. What components of more familiar teams can we utilize within our existing systems? Can we proxy some of the features of more familiar teams? Can technology help us apply the lessons learned for the benefit of everyone?
In part 2 of this blog, we dive deep into these questions and examine some of the real-world strategies to support our teams to perform at their very best. Stay tuned; you won’t want to miss it!
Here at Incision, we’re dedicated to writing blogs that inspire conversation, bring teams closer together and educate in a dynamic way. When we learn together we grow together, so join the conversation!